Often called “gel injections,” HA is a synthetic version of the fluid naturally found in healthy joints.
Scientific Evidence (2026):
“PRP showed significantly better functional scores at 6 and 12 months compared to simple intra-articular injection of HA. Specifically, PRP can improve WOMAC scores, VAS pain scores, and the IKDC index, enhancing a patient’s health status more effectively over the long term.” > — The efficacy and safety of PRP and HA in the treatment of knee osteoarthritis, Frontiers (2026).
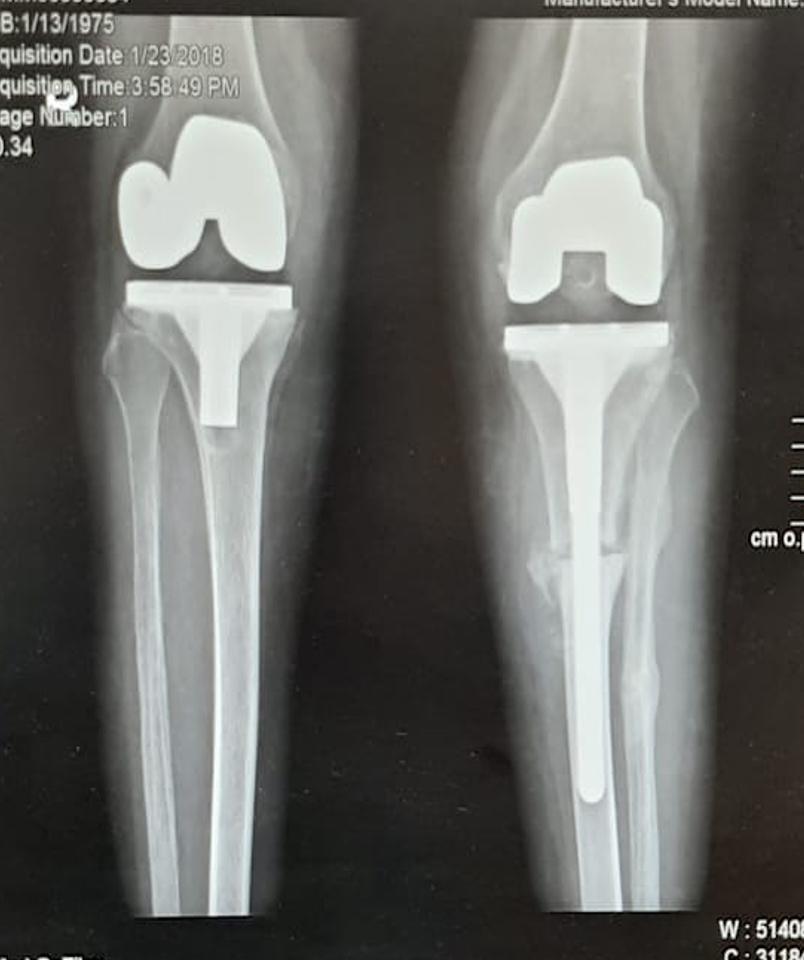
1. Total Hip Replacement
Replacing the ball-and-socket joint partially destroyed with artificial material, restoring mechanical movement and relieving pain.
2. Surgery to Resurface the Hips
An alternative to complete replacement that preserves more natural bone and is often suitable for younger, active patients.
3. Bilateral Replacement of the Hip
A procedure where both hip joints are replaced in one surgery due to severe pain or injury on both sides.
4. Hip Revision
A corrective surgery performed to repair or replace an already implanted hip joint that has worn out or failed.
5. Minimally Invasive Hip Replacement
A modern technique using smaller incisions, causing less tissue damage, faster recovery, and shorter hospitalization.
| Feature | Hyaluronic Acid (HA) | Platelet-Rich Plasma (PRP) |
|---|---|---|
| Primary Goal | Lubrication & Cushioning | Inflammation control & Repair |
| Source | Laboratory-made | Your own blood (Autologous) |
| Duration of Relief | ~6 Months | 9–12+ Months |
| Best Stage | Early/Mild OA | Mild to Moderate OA |
| Safety | High (rare local flares) | High (minimal risk of reaction) |